 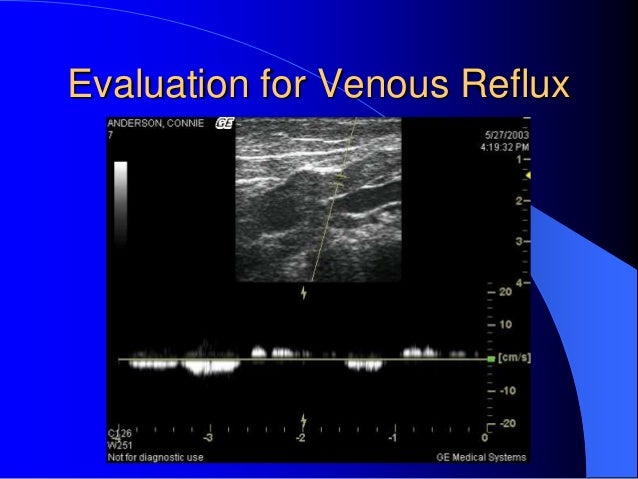
However, the preferred provocation maneuver is the use of a cuff inflation-deflation technique with rapid cuff deflation in the standing position. Prolonged reversal flow after augmentation suggests venous reflux. Downward pressure is transmitted down and through the dysfunctional valves until it reaches the functioning valve. 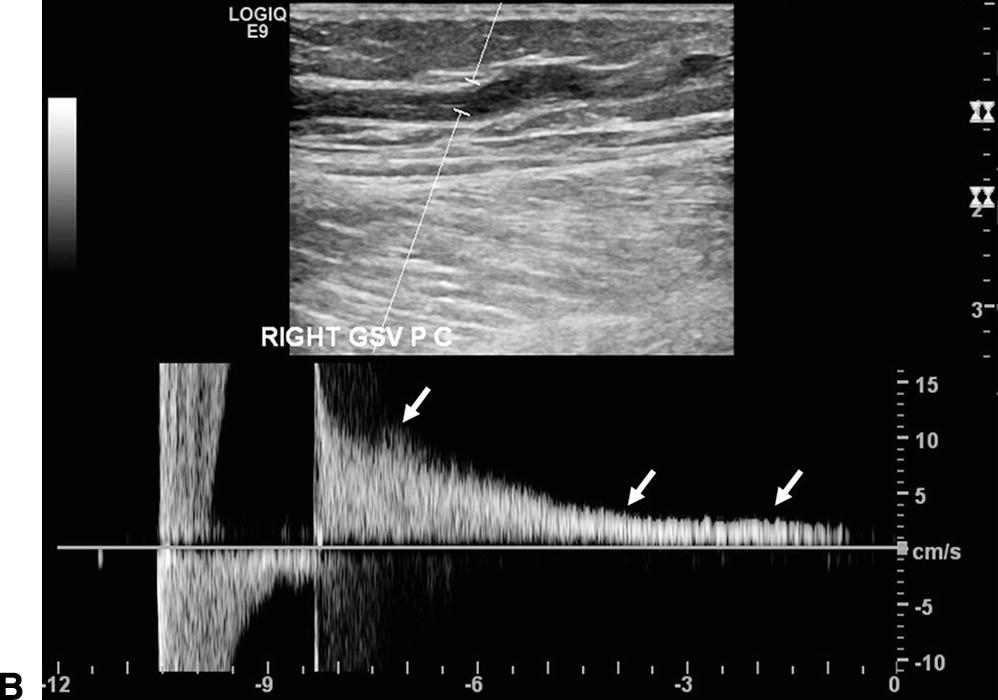 
The primary goal of this test is to evaluate the flow characteristics and valve functions in the central vessels. The Valsalva maneuver increases intra-abdominal pressure. Although reverse flow can be detected without the provocation maneuver, the Valsalva maneuver or augmentation by compressing the calf can be used to confirm venous reflux. Venous reflux is assessed in the reverse Trendelenburg position. Any significant reverse flow toward the foot is considered venous reflux ( Fig. Venous reflux is detected by the direction of flow. Diagnosis of venous reflux Diagnosis of venous reflux Iliac vein non-thrombotic stenosis can be seen by the increased blood velocity from DUS at the iliac veins ( Fig. Compressibility is the most reliable way of diagnosing an intraluminal thrombus and this technique is performed in a short-axis view. However, the major limitation of this maneuver is the variability of the force of the compression. Blunting of augmentation suggests obstruction. This maneuver is used to confirm the patency of the vein segment. When performing a compression, it is best to squeeze and hold for approximately 0.25 second and then release. Augmentation by applying a moderately firm squeeze over the calf to increase flow moving centrally can be evaluated in normal veins. Spontaneous flow should be evaluated in a supine or slight reverse Trendelenburg position, not standing position. In addition, nearly constant high velocity flow without significant respiratory changes indicates a proximal stenosis or occlusion ( Fig. An absence of spontaneous flow may indicate an obstruction either proximal or distal to the area of examination. Small veins, such as calf veins, usually do not show spontaneous flow because of their size. Normal flow stops during inspiration and returns during expiration because of the increased intra-abdominal pressure during inspiration. This flow reflects respiratory changes ( Fig. Large veins such as the inferior vena cava, iliac, femoral, and popliteal vessels show spontaneous blood flow at rest. The diagnosis of venous obstruction can be inferred from the absence of flow, blunted augmentation, the presence of an echogenic thrombus within the vein, or failure of the vein to collapse by a compression maneuver ( Fig. Pelvic CVI, defined as retrograde flow in the gonadal and internal iliac veins, is the underlying cause of pelvic congestion syndrome, a common cause of disabling chronic pelvic pain in women of child-bearing age, and endovascular embolization has become the treatment of choice for this syndrome. Even though such lesions can be found in half of the asymptomatic population, the clinical sequelae, such as DVT or CVI, are only observed in approximately 3% to 5% of patients. An Iliac vein compression syndrome (or May-Thurner syndrome) is a clinical condition that occurs as a result of compression of the left iliac vein between the right iliac artery and the fifth lumbar vertebrae. In contrast, non-thrombotic iliac vein lesions, such as stenosis, can also cause CVI. This can be treated with a stent, but the patency of this type of lesion is inferior to that of non-thrombotic occlusion. This type of occlusion is categorized as a thrombotic occlusion. After DVT, only 20% to 30% is fully recanalized, and residual obstruction is associated with severe CVI. Obstruction in the iliac vein plays a significant role in CVI. The veins of the pelvis consist of three major vessels: the external iliac vein, the internal iliac vein, and the common iliac vein. VENOUS ANATOMY AND ITS VARIATIONS VENOUS ANATOMY AND ITS VARIATIONS Postthrombotic syndrome after deep vein thrombosis (DVT) also causes venous hypertension due to the remaining obstruction of the venous flow and valvular reflux due to valve damage. This is called ambulatory venous hypertension. If valves in the perforator veins are incompetent, the high pressures generated in the deep veins by calf-muscle contraction can be transmitted to the superficial system and to the microcirculation in skin. However, in a patient with CVI, the decrease in venous pressure with leg movements is attenuated. In a subject with competent venous valves, this pressure decreases to less than 30 mmHg during ambulation. The venous pressure of the foot vein in the standstill position without skeletal muscle contraction is as high as 80 to 90 mmHg. The main pathophysiological cause of the clinical manifestation of CVI of the lower extremities is ambulatory venous hypertension, which is caused by venous valve reflux, venous flow obstruction, or both. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
